

What is a multiparametric MRI of the prostate?
Early detection of prostate cancer is now safer and less invasive than ever before. At our practice, we rely on multiparametric MRI (mpMRI)—currently the most advanced and precise method for examining the prostate gland.
Thanks to high-resolution cross-sectional images and functional analyses, we achieve a level of diagnostic certainty that far exceeds that of conventional methods. Whether for preventive care, in cases of rising PSA levels, or for precise treatment planning: We offer you peace of mind through state-of-the-art technology and certified, specialized expertise, so you can be confident about your health—quickly, painlessly, and without radiation exposure.
Since prostate cancer is the most common form of cancer among men in Germany and often causes no symptoms in its early stages, accurate early detection is the key to successful and minimally invasive treatment.
However, elevated PSA levels or urinary problems are often caused by benign prostatic hyperplasia (BPH) or inflammation (prostatitis). These conditions can also be reliably diagnosed using MRI. This provides you with a reliable diagnosis that serves as the basis for your further, targeted treatment.
The benefits of our practice
- Quick appointment scheduling
- Short examination time (approx. 16 minutes)
- Modern MRI technology
- High diagnostic accuracy: guideline-based examination protocols, Q2-certified evaluation, and double-reading
- Personalized care in a welcoming atmosphere
- In-person or telephone discussion of test results
When is a prostate MRI recommended?
mpMRI is used when conventional diagnostic methods (PSA level, digital rectal exam, or ultrasound) reveal abnormalities that require further investigation. Die Hauptgründe für eine Untersuchung sind:
- Elevated/rising PSA level: Suspected cancer when the cause of the increase is unclear
- Abnormal findings on physical examination or ultrasound, with suspicion of carcinoma
- Negative biopsy with persistent suspicion of cancer: When no tumor is found despite a tissue sample, but PSA levels continue to rise.
- Active Surveillance: For known, low-grade tumors, multiparametric MRI is used for close monitoring to detect disease progression at an early stage.
- Precise Cancer Screening: For men with an increased family history of cancer or who want the utmost peace of mind, mpMRI offers a level of screening quality that far exceeds that of conventional physical examination or ultrasound. It serves as a “safety net” to detect tumors requiring treatment at a stage when they are still highly treatable.
- Treatment planning: To accurately determine the extent of the tumor prior to surgery or radiation therapy.
Prostate cancer (PIRADS-4 classification)
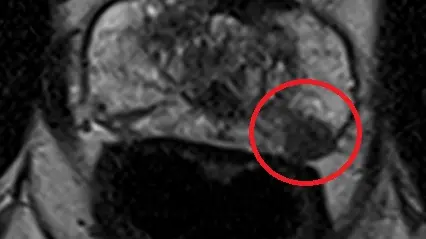
T2 weighting
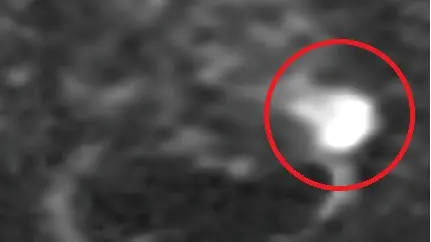
Diffusion weighting

Contrast-enhanced imaging
Procedure and Conduct of a Prostate MRI
Below, we will explain the examination process step by step.
1. Preparing for the examination
- Information and guidance before the MRI exam:
- Discussion of your current symptoms
- Submission of any previous test results (e.g., PSA level, ultrasound, biopsy)
- Discussion of pre-existing conditions and, if applicable, implants
- Identification of any contrast agent intolerances
Because MRI uses a strong magnetic field, there must be no metal objects on or inside the body (e.g., jewelry, watches, hearing aids, bank cards). Implants such as pacemakers must be checked in advance.
No special preparation is necessary. You can eat and drink as usual.
However, you should come to the appointment with someone accompanying you, as you will be given a medication (Buscopan) during the MRI to improve image quality, which in rare cases can cause side effects such as blurred vision.
2. Positioning within the MRI scanner
For the exam, you will lie comfortably on your back on the examination table. The table will move slowly into the MRI machine (your head will remain outside the machine during the exam), so you can lie still and relaxed throughout the entire procedure. A prostate MRI takes about 16 minutes at our practice.
3. The actual MRI scan
An MRI uses a strong magnetic field and radio waves—without X-rays. During the exam, you will hear loud knocking or humming noises. For this reason, you will be given earplugs or headphones. In accordance with guidelines, you will also receive a well-tolerated contrast agent and Buscopan (which slows natural bowel movements) through a vein in your arm.
The examination includes various image sequences (multiparametric), including:
- High-resolution T2-weighted images (assessment of anatomy)
- Diffusion-weighted sequences (assessment of cell density)
- Dynamic contrast-enhanced imaging (assessment of blood flow)
This combination allows for a highly accurate assessment based on internationally recognized criteria (the PIRADS scoring system).
4. After the examination
The exam will be completed in about 16 minutes, and you will receive the images on a CD and via a QR code. If you have been given Buscopan, you should not drive a car or operate heavy machinery on that day. Otherwise, you can resume your normal activities immediately after the exam.
The MRI images are carefully interpreted by our highly specialized radiologists (Q1/Q2 certification by the German Radiological Society). The written report is sent promptly (usually within 48 hours) to your treating physician. In addition, you will receive a preliminary consultation regarding the findings and access to your examination images, including the report, via our digital patient portal.
If you have any questions about prostate MRI, our team is always happy to assist you. We will guide you through the entire examination with expertise and sensitivity.
What are the benefits of a prostate MRI?
Choosing an mpMRI at our practice offers you, as a patient, significant advantages:
- Unparalleled accuracy: The test detects clinically significant tumors with significantly greater reliability than conventional screening methods.
- No radiation exposure: The examination uses magnetic fields, not X-rays.
- Targeted biopsy instead of a “shotgun approach”: If a tissue sample needs to be taken, our MRI data provides the exact coordinates for a fusion biopsy. This increases the likelihood of directly targeting malignant areas and reduces the number of samples required.
- Avoiding overdiagnosis and unnecessary biopsies: Benign changes can be more easily distinguished from aggressive tumors, saving you unnecessary worry and treatment.
- Non-invasive and painless: The examination is performed without any direct intervention in the body.
Enlarged prostate
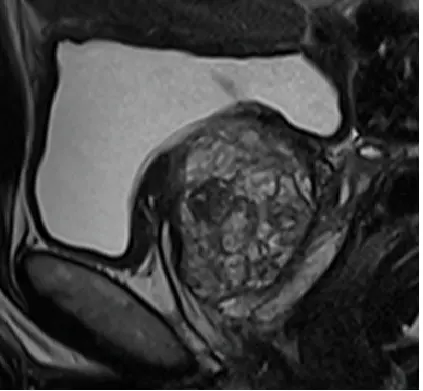
T2w sagittal
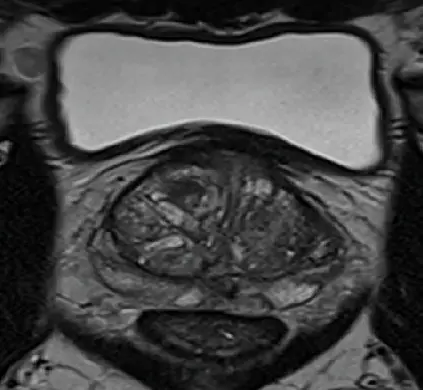
T2w axial
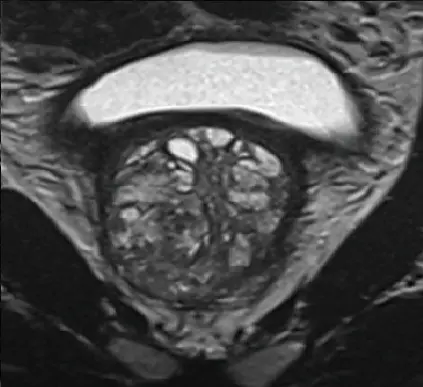
T2w coronal
Will health insurance cover the costs?
Private health insurance plans usually cover the full cost of mpMRI.
Schedule your appointment online right here!
Unfortunately, statutory health insurance plans generally do not yet cover the cost of this examination, as mpMRI—despite its importance and its inclusion in the S3 guideline on “Prostate Cancer”—has not yet been added to the list of services covered by statutory health insurance (EBM). If you have statutory health insurance, the following options are available to you:
- As a self-pay patient (we would be happy to provide you with a cost estimate).
- As part of a so-called selective contract. Some health insurance providers now offer their members access to this modern diagnostic procedure through a so-called selective contract. This means they cover the cost of the examination. Is your health insurance provider one of them?More information.
- Request for reimbursement from your statutory health insurance provider. We are happy to assist you with this and can provide you with an application form. Please feel free to contact us.
Here are some frequently asked questions about prostate MRI scans.
The prostate is a walnut-sized gland (known as the prostate gland) located below the bladder in men. It produces an important component of seminal fluid and is therefore crucial for fertility. Since it surrounds the urethra and acts as a muscular valve to separate the urinary and seminal pathways, a prostate condition—such as inflammation, enlargement, or prostate cancer—can affect urine flow.
Multiparametric MRI (mpMRI) of the prostate is a modern, high-resolution imaging technique used for the early detection and accurate diagnosis of prostate cancer. It combines various MRI sequences to distinguish benign changes from clinically significant tumors. mpMRI plays a key role prior to a prostate biopsy and in cases of unclear PSA levels.
No. A prostate mpMRI is a non-invasive and painless procedure. During the MRI, you will lie comfortably on an examination table. The only sound you will hear is the typical loud knocking noise, for which you will be provided with ear protection.
In most cases, no special preparation is required. Before the examination, we will ask about any medical devices you may have, such as a pacemaker, or any relevant pre-existing conditions. Depending on the nature of the examination, it may be necessary to adjust certain medications at short notice. You will receive detailed instructions prior to your appointment.
Unfortunately, statutory health insurance plans generally do not cover the cost of prostate MRI scans at this time, as the procedure—despite its importance and firm inclusion in the S3 guideline on “Prostate Cancer”—has not yet been added to the GKV’s (EBM) list of covered services. In this case, you may opt to undergo the examination as a self-pay patient. We would be happy to advise you transparently and individually on the potential costs and reimbursement options. In addition, it has recently become possible to undergo mpMRI of the prostate under a so-called selective contract with various statutory health insurance providers. This means they cover the cost of the examination. Is your health insurance provider included?
Find more information here!
No. An MRI uses a strong magnetic field—there is no exposure to X-rays or ionizing radiation. The procedure is therefore considered particularly gentle.
In many cases, a normal mpMRI can help avoid an unnecessary biopsy. However, if the scan reveals suspicious areas, it enables a targeted MRI-guided or fusion biopsy. This increases the success rate and improves the diagnosis of prostate cancer.
Yes. The diagnostic value of prostate MRI depends largely on state-of-the-art equipment, standardized examination protocols, and the expertise of specialized radiologists (Q1/Q2 certification in prostate MRI interpretation by the German Radiological Society). Structured interpretation according to international PI-RADS criteria is essential for reliable diagnosis. You’ll find all these factors right here in our practice!
Prostatitis (inflammation of the prostate) should be evaluated by a urologist. Typical symptoms include pain in the pelvic area, difficulty urinating, or fever. Treatment depends on the cause; antibiotic therapy is often prescribed (e.g., for bacterial inflammation). In cases of nonbacterial prostatitis (chronic pelvic pain syndrome), however, symptom relief can also be achieved through heat therapy, physical therapy, relaxation exercises, and, if necessary, medication. There is also a form of prostatitis that is symptom-free (asymptomatic prostatitis).
Benign prostatic hyperplasia (BPH) is a common cause of urinary symptoms. Depending on the severity, treatment options may include medication, minimally invasive procedures, or surgery. Early diagnosis, for example via MRI, can help rule out other causes such as prostate cancer and enable targeted, follow-up urological treatment.
No. At our practice, prostate MRI scans are performed without inserting a coil into the rectum.
Instead, we use state-of-the-art MRI technology with special external receiver coils placed on the pelvic area. This allows us to produce high-quality, detailed images of the prostate without the need for an additional rectal examination.
After a prostate biopsy, you should generally wait about 4 to 6 weeks before having a prostate MRI. The tissue samples taken cause minor bleeding in the prostate, which may be visible on the MRI and make it difficult to interpret the results. Once enough time has passed, we can evaluate the images much more reliably.
In some cases, the exact timing can be determined on an individual basis in consultation with the treating physician.
In most cases, we use a contrast agent for prostate MRI, which is administered through a vein in the arm. This allows for a more accurate assessment of blood flow and tissue structure in the prostate.
The advantage is that suspicious areas can often be identified more easily and distinguished more reliably from benign changes. This increases the diagnostic value of the examination.
The MRI contrast agent used is generally very well tolerated. We will determine on a case-by-case basis whether to use it in your case prior to the examination.
Yes, in most cases, a prostate MRI is perfectly feasible even for patients with claustrophobia. Our MRI machines have a particularly wide opening, so many patients find the exam much more comfortable. In addition, you’ll be connected to our team via an intercom system throughout the entire exam.
If you still feel very anxious about the examination room, we can discuss additional ways to help you feel more comfortable before the exam.
PI-RADS is a standardized scoring system for prostate MRI. Radiologists use it to describe how abnormal an area of the prostate appears on an MRI scan and how likely it is that this area could conceal a significant change in the prostate that requires treatment.
Ratings are given on a scale of 1 to 5:
- PI-RADS 1–2: A significant lesion is highly unlikely.
- PI-RADS 3: Indeterminate finding – follow-up; further evaluation may be advisable.
- .PI-RADS 4–5: A significant finding is increasingly likely.
Important: PI-RADS is not a definitive diagnosis, but rather an assessment of the imaging findings. The next steps will always be determined in consultation with your treating urologist.
Standard prostate screening typically consists of a PSA blood test and a digital rectal exam performed by a urologist. While these tests can provide indications of abnormalities, they do not provide direct images of the prostate.
In contrast, prostate MRI produces highly detailed images of the entire prostate. This allows changes in the tissue to be detected earlier and more accurately, and their location to be pinpointed with precision. Another advantage is that areas that are difficult to reach during a digital rectal exam—such as the front part of the prostate or the tip—can still be clearly assessed using MRI.
If a tissue sample is needed, MRI can also help pinpoint suspicious areas, allowing for more precise planning of a potential biopsy.
The written report of your prostate MRI is usually available promptly (typically within 48 hours). We will then discuss the results with you as soon as possible.
In addition, the results will be sent to your treating urologist. He or she will discuss the next steps with you and work with you to decide whether, for example, a follow-up visit, further testing, or, if necessary, a targeted biopsy is appropriate.
The Q1 and Q2 certifications are quality certifications issued by the German Radiological Society (DRG) for radiologists who interpret prostate MRIs. They confirm specialized training and experience in evaluating this type of examination.
- Q1 Certification: Evidence of structured continuing education and experience in interpreting prostate MRI scans.
- Q2 Certification: A higher qualification level requiring extensive experience and a larger number of evaluated studies.
For you as a patient, this means that the examination and interpretation of results are performed by specially trained radiologists in accordance with high-quality standards.
A prostate MRI may be recommended if you have an increased personal risk or if your screening results are abnormal. This includes, for example, elevated or rising PSA levels, an unclear digital rectal exam by a urologist, or abnormal results from previous examinations.
Even if there is a family history of the disease—for example, if close relatives have had prostate cancer—an MRI may be useful for early and more accurate diagnosis.
The advantage of an MRI is that it provides detailed images of the prostate without causing pain or exposing the patient to radiation, and can detect potential changes at an early stage.
For the examination, you will usually be given a medication (Buscopan) that reduces bowel movements and thus improves image quality. After taking this medication, you should not drive on the day of the examination.
We therefore recommend that you arrange for someone to drive you home or use public transportation.
References:
S3-Leitlinie Prostatakarzinom
https://register.awmf.org/assets/guidelines/043-022OLl_S3_Prostatakarzinom_2025-08.pdf


