Cardiac MRI
Magnetic Resonance Imaging of the Heart
Using modern MRI technology with high temporal and spatial resolution, it is possible to produce both still cross-sectional images of the heart and moving images of the beating heart. MRI thus allows us to assess the anatomy, function, and pathological changes in the heart’s structures.
Unlike cardiac catheterization, computed tomography, or scintigraphy, MRI provides high-contrast images of the heart without exposing the patient to radiation. Its advantage over echocardiography is that image quality is not dependent on the examiner or on the patient’s physical characteristics (height, chest circumference, lung volume, etc.).In what situations is cardiac MRI recommended?
Cardiac MRI can provide answers to questions regarding the anatomy of the heart, the functional assessment of the heart chambers and valves, as well as diseases of the heart muscle. It can provide information on past heart attacks, inflammatory changes in the heart muscle or pericardium, (rarer) neoplastic changes, as well as structural changes in the heart muscle (cardiomyopathies). A stress MRI of the heart allows for the non-invasive detection of exercise-induced blood flow abnormalities in the heart muscle and is therefore an alternative to cardiac catheterization. For this procedure, a medication (adenosine) is administered through an arm vein over a 4-minute period, which temporarily and controllably increases cardiac output.
In summary, MRI is indicated for the following conditions or suspected diagnoses:
- Inflammation of the heart muscle or pericardium (myocarditis, pericarditis)
- Heart valve defect
- Congenital heart defects
- Coronary heart disease: Detection and extent of a heart attack (myocardial scarring), exercise-induced reduced blood flow to the heart muscle (stress MRI)
- Different forms of heart muscle disease (cardiomyopathy [CM]): hypertrophic CM, dilated CM, arrhythmogenic right ventricular CM (ARVC), metabolic CM, Fabry disease, amyloidosis…
- Heart tumors/masses, blood clots in the heart
- Disease of the aorta or the central pulmonary arteries
Before the examination
Before any MRI scan, you must remove all metal objects (watches, credit cards, jewelry, hearing aids, eyeglasses). If possible, avoid wearing clothing with many metal accessories (buttons, zippers, underwire bras). For a cardiac examination, you must expose your upper body before the exam so that the ECG electrodes can be placed.
If you have a known intolerance to contrast agents, please inform the staff (radiologic technologists or physicians) in advance. An intolerance to X-ray contrast agents (iodine-based contrast agents) is not a contraindication for the administration of contrast agents during an MRI (gadolinium-based contrast agents).
If you are scheduled to undergo a stress cardiac MRI, there are certain foods and medications that you must not consume for 24 hours prior to the exam, as they can interfere with the results. These include:
- No coffee, tea, cocoa, energy drinks, or cola
- No chocolate, fruit gummies, or bananas
- No beta-blockers (e.g., metoprolol, Beloc, carvedilol, bisoprolol...)
- No medications containing nitrates (Nitrolingual, Molsidomin, ISDN, Corvaton)
- No medications containing theophylline
Procedure for the examination
Under a standard protocol, a cardiac examination takes an average of 45 minutes. A cardiac stress test takes approximately 50–60 minutes, primarily because of the increased time required to monitor the patient during the 4-minute “stress phase.”
The patient lies on their back on the examination table. Before the examination begins, ECG electrodes are attached to the chest to capture motion-free images of the beating heart. In addition, a narrow, very lightweight coil is placed on the chest to optimize image quality. If intravenous contrast administration is necessary for the specific examination, an IV catheter is inserted into a vein in the arm. Since every MRI examination involves significant noise, each patient is provided with headphones. The staff can use these to communicate with the patient even during the examination. The patient is also given an emergency bell to hold. The patient is then wheeled into the machine, and the examination begins.
Patients who suffer from a fear of confined spaces (claustrophobia) may be given a sedative upon prior request. However, these patients must inform the staff in advance and may only come to the examination accompanied by someone else.
To avoid capturing breathing artifacts, the individual image sequences are acquired during several breath-hold periods. To this end, the patient is repeatedly given breathing instructions involving breath-hold phases of 10–15 seconds.
During a standard cardiac MRI, the patient is administered a small amount of contrast agent intravenously about halfway through the examination. The contrast agent used in MRI is generally very well tolerated and, on average, causes even fewer (allergic) side effects than iodine-containing contrast agents used in computed tomography or cardiac catheterization. Most patients do not notice the administration of the contrast agent at all, or at most feel a cool, flowing sensation in their arm during the injection.
After the examination
Once the examination is complete, no further monitoring of the patients is necessary, so they may leave the office after receiving their examination records (CD).
The results of the examination are interpreted by radiologists who are trained and experienced in cardiac imaging (holders of the German Radiological Society’s Q-certificate for cardiac imaging) to a high professional standard. The written report is sent promptly to the referring physician.
Stress perfusion MRI of the heart
If a cardiac stress test is required to diagnose a blood flow disorder in the heart muscle (coronary artery disease [CAD]), additional patient preparation is necessary: To monitor the patient’s vital signs during the pharmacological stress sequence, a blood pressure monitor and a pulse oximeter are attached prior to the test, in addition to the ECG, to measure heart rate and blood oxygen saturation. During the injection of the stress medication (adenosine), a physician is always present at the equipment, monitoring vital signs and maintaining verbal communication with the patient.
During the 4 minutes of the stress injection, the patient’s heart is subjected to simulated physical stress, causing an increase in heart rate and breathing rate (similar to running in place). Some patients may experience a slight feeling of pressure in the chest or a sensation of pressure or heat in the head during this time. This is normal and not dangerous. In rare cases, other symptoms such as significant changes in blood pressure, dizziness, shortness of breath, or heart rhythm disturbances may occur. During the first 2 minutes of the stress phase, the patient remains outside the tube and can speak directly with the physician standing by the machine about any physical sensations. During the following 2 minutes, the actual measurement takes place inside the machine with an additional injection of contrast agent. Immediately after the stress test, the patient is moved out of the machine and their vital signs are checked again.
Once the adenosine injection is completed, the symptoms subside completely within a few minutes due to the drug’s very short duration of action. The MRI examination then continues with the remaining standard cardiac sequences.
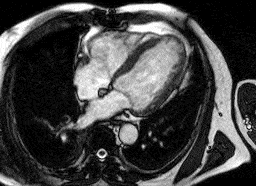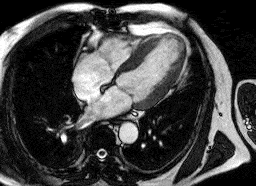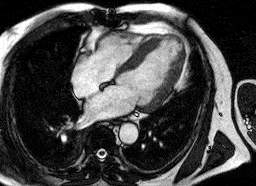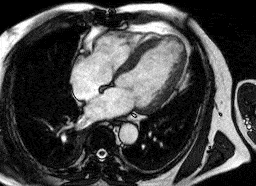
Heart attack
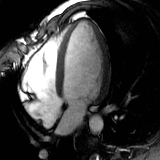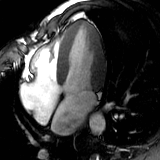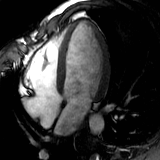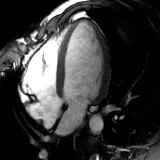
Normal heart
Which patients should not undergo a cardiac MRI?
In general, patients with implanted pacemaker systems (cardiac pacemakers, implantable defibrillators, brain pacemakers, neurostimulators) or other electronic implants (insulin pumps, etc.) should not undergo MRI examinations. Pregnant women should not receive either contrast agents or adenosine and, as a rule, should therefore not undergo standard cardiac MRI or stress MRI. Patients with artificial heart valves and severe cardiac arrhythmias are generally not suitable candidates for cardiac MRI due to the expected artifacts.
Patients with a known intolerance to MR contrast agents (gadolinium) can only undergo native sequences, which means that no conclusions can be drawn regarding inflammatory or ischemic changes. The same applies to patients with known renal impairment and dialysis patients.
There are additional exclusion criteria/contraindications for a stress MRI of the heart:
- Common chronic obstructive pulmonary diseases: COPD, chronic bronchitis, asthma
- Generally low blood pressure: systolic pressure below 90 mm Hg
- Severe cardiac arrhythmias: AV block, sick sinus syndrome
- Severe aortic valve stenosis
- Severe heart failure
- Recent heart attack (less than 1 week ago), unstable angina
- Known main trunk stenosis
- Current dipyridamole therapy or use of methylxanthines
- After a liver transplant


